Gram stain: The Gram stain, is a laboratory staining technique that
distinguishes between two groups of bacteria that have differences in
the structure of their cell walls. Standard bacterial taxonomy makes a
distinction between Gram-negative bacteria, which stain red/pink and
the Gram-positive bacteria, which stain blue/purple. Different
antimicrobial agents are directed specifically at gram-positive
bacteria and gram-negative bacteria.
Slide coagulase test: The slide Coagulase test
detects bound coagulase (clumping factor). This type of coagulase is
attached to the bacterial cell walls (surface). This test is usually
performed on a glass slide.
Tube Coagulase test: The coagulase test is used
to differentiate Staphylococcus aureus from coagulase-negative
staphylococci. The test uses rabbit plasma that has been inoculated with
a staphylococcal colony. The tube is then incubated at 37 degrees
Celsius for 1-1/2 hours. If negative, then incubation is continual up to
24 hours. This test detects free coagulase (coagulase that is released
by bacterial cells into culture).
·
Positive (i.e., the suspect colony is S. aureus). The serum will
coagulate, resulting in a clot (sometimes the clot is so pronounced that
the liquid will completely solidify).
·
Negative, the plasma remains liquid. A negative result may
be S. epidermidis.
Catalase test: The catalase
test is used to differentiate some bacterial species. The test is done
by placing a drop of hydrogen peroxide on a microscope slide. Using an
applicator stick, a small portion of a colony is then added to a drop of
hydrogen peroxide drop.
- If bubbles or froth forms, the organism is
said to be catalase-positive.
Staphylococci and micrococci are catalase-positive
- If no bubbles form, the organism is catalase-negative.
Streptococci and Enterococci are catalase-negative
Tube Coagulase test: The coagulase test is used
to differentiate Staphylococcus aureus from coagulase-negative
staphylococci. The test uses rabbit plasma that has been inoculated with
a staphylococcal colony. The tube is then incubated at 37 degrees
Celsius for 1-1/2 hours. If negative, then incubation is continual up to
24 hours. This test detects free coagulase (coagulase that is released
by bacterial cells into culture).
·
Positive (i.e., the suspect colony is S. aureus). The serum will
coagulate, resulting in a clot (sometimes the clot is so pronounced that
the liquid will completely solidify).
·
Negative, the plasma remains liquid. A negative result may
be S. epidermidis.

PYR test: the PYR test is a qualitative
procedure for determining the ability of streptococci to enzymatically
hydrolyze L-pyrrolidonyl- β-napthylamide (PYR). A positive PYR tests
allows for the presumptive identification of group A streptococci (Streptococcus
pyogenes) and group D Enterococci.
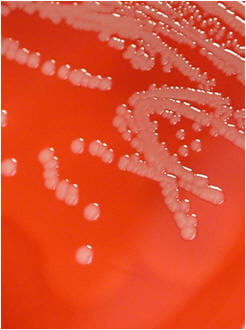
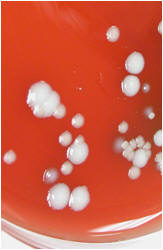
Non-hemolytic (γ-hemolysis): If an organism
does not induce any hemolysis on a blood agar plate, it is said to
display gamma or no hemolysis. The agar under and around the colony is
unchanged.
Alpha
hemolysis (α-hemolysis):
Alpha hemolysis is the incomplete lysis of the red blood cells around
and under the colonies on a blood agar plate. This area appears dark and
greenish. Streptococcus pneumoniae and a group of streptococci (Streptococcus
viridans or viridans streptococci) found in oral flora display alpha
hemolysis.
Beta
hemolysis (β-hemolysis): Beta hemolysis is the complete lysis of the
red blood cells around and under the colonies on a blood agar plate.
This area appears transparent. Streptococcus pyogenes displays
beta hemolysis and is often called Group A beta-hemolytic strep (GABHS).
PYR test: the PYR test is a qualitative
procedure for determining the ability of streptococci to enzymatically
hydrolyze L-pyrrolidonyl- β-napthylamide (PYR). A positive PYR tests
allows for the presumptive identification of group A streptococci (Streptococcus
pyogenes) and group D Enterococci.

















![]()


![]()

![]()
![]()
![]()

![]()
![]()

![]()
![]()

